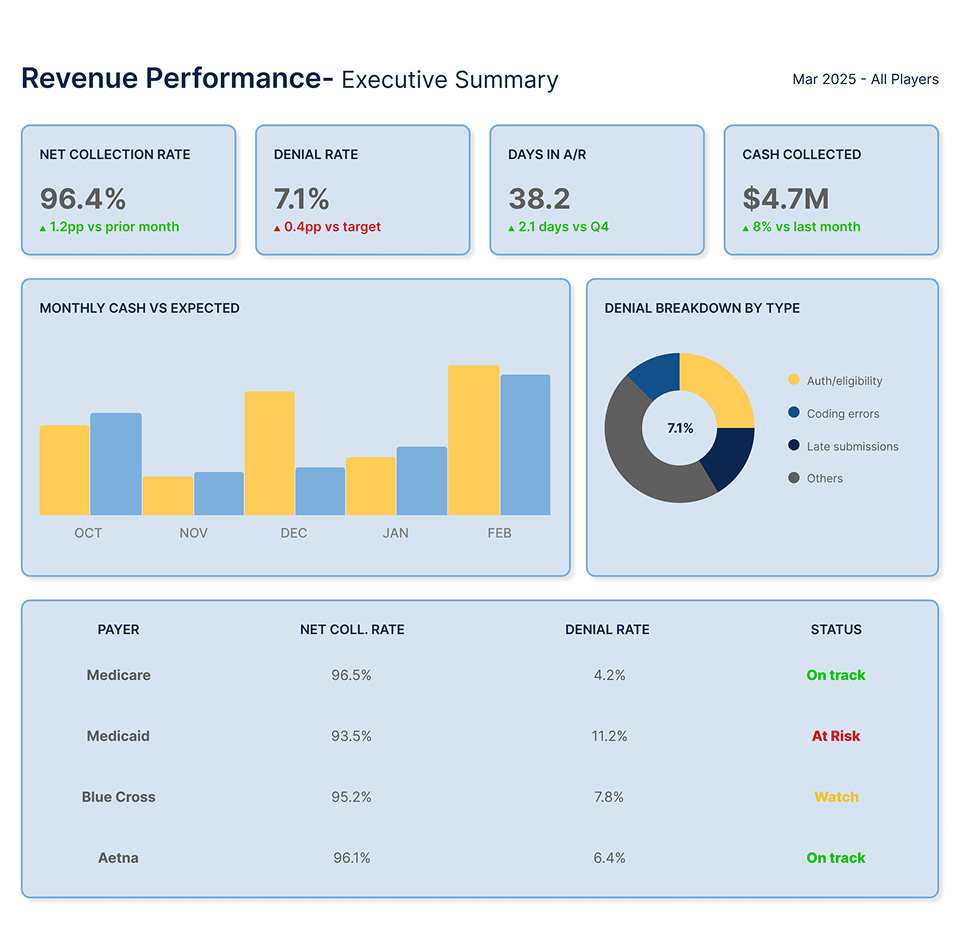
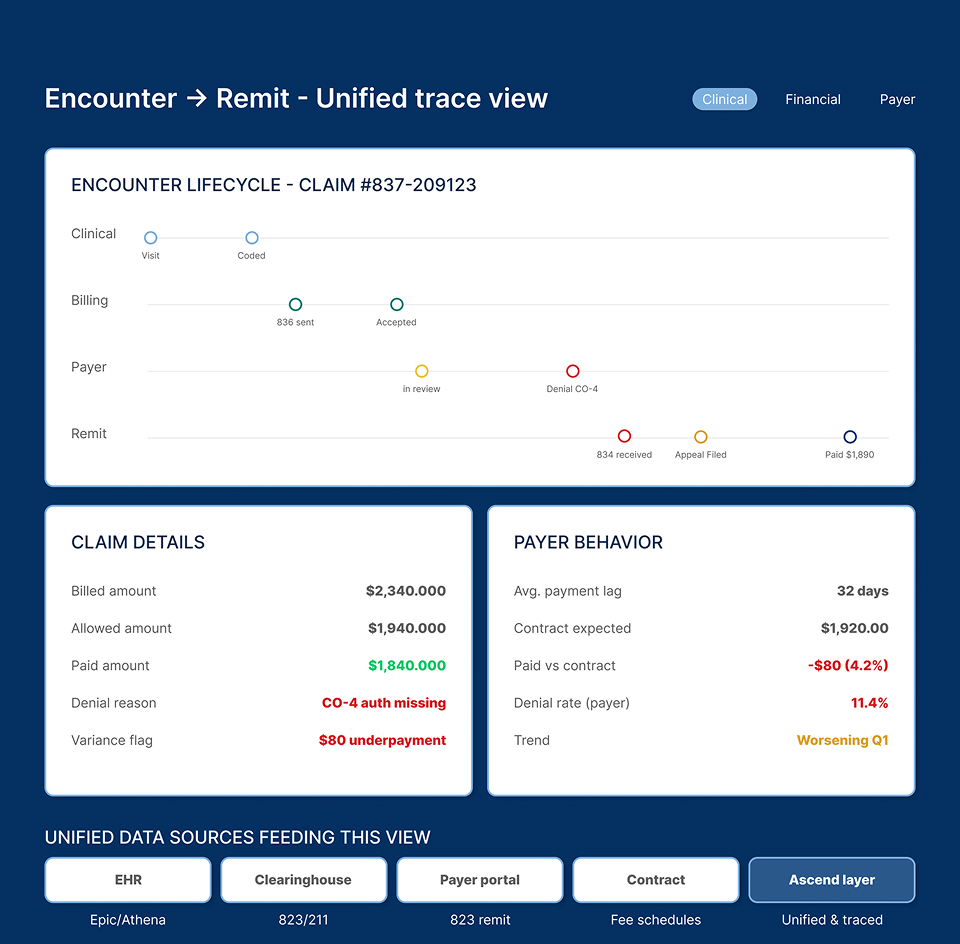
We unify clinical, financial, utilization, post-acute, and RPM data from EHRs, billing platforms, clearinghouses, and payer responses so analytics and AI operate on consistent, trusted information.
Well-structured pipelines and standardized layers make reporting, forecasting, and AI use cases possible without repeated engineering effort.
Every metric, feature, and output ties back to its source with clear logic, governance, and documentation built in.
Most healthcare organizations already have powerful systems in place - Epic/Athena, claims platforms, payer portals, contract tables but the data between them doesn’t naturally align.
Clinical events, billing workflows, remittances, and payer behavior arrive in different formats, at different times, with inconsistent definitions. The result is fragmented visibility, slow reporting cycles, and limited ability to build scalable analytics on top.